Treating Preventing Chronic Pain
Treating and Preventing Chronic Pain and Addiction
By James Fricton DDS, MS
What pain conditions does MN Head & Neck Pain Clinic Treat?
The pain specialists at the Minnesota Head and Neck Pain Clinic (MHNPC) provide interdisciplinary transformative care for patients of all ages with an acute to chronic TMJ disorder, facial, head and neck pain conditions.
Types of pain relief treatment people seek us out for include:
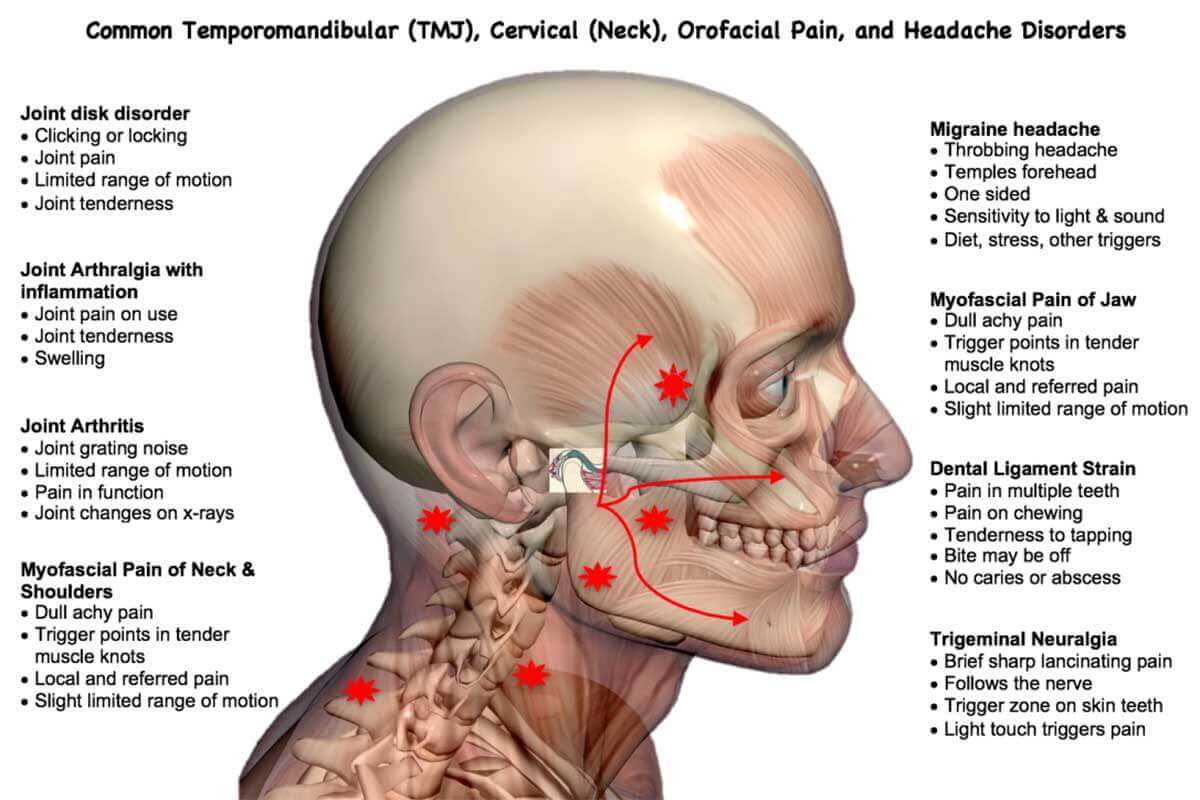
- Temporomandibular muscle and joint (TMJ) disorders with pain, clicking and locking in the jaw
- Facial and jaw pain disorders including trigeminal neuralgia, orofacial nerve injuries, and other neuralgias
- Sleep Apnea, snoring, and orofacial airway disorders
- Headaches including migraine, tension headaches, mixed headaches, and cluster headaches
- Neck and shoulder pain including cervical muscle and joint pain
- Oral and dental pain including tooth pain, burning mouth and tongue, and sensitive teeth
- Orofacial movement disorders such as bruxism, dyskinesias, and tremors
What is chronic pain?
Chronic pain is the top reason to seek care, the #1 cause of disability and addiction, and the primary driver of healthcare utilization, costing more than cancer, heart disease, and diabetes. Studies have shown that more than half of the persons seeking care for pain conditions at 1 month after it begins still have pain 5 years later despite treatment.
The development of chronic pain is often due to many factors including:
- There are many symptoms that confuse the pain causes, especially for bruxism diagnostic process.
- There is often lack of identifying and treating the multiple overlapping pain conditions that cause an array of symptoms
- Risk factors that can lead to treatment failure and chronic pain cycle that perpetuates pain
- Need patient training to reduce risk factors in addition to treatment of the condition
How do we Treat Patients with Pain Conditions?
Although treatments such as physical therapy, medications, injections, and splint can provide relief of pain conditions, research shows that patient engagement in self-management such as cognitive-behavioral therapy (CBT), therapeutic exercise, and mindfulness-based stress reduction can activate and empower patients to reduce risk factors to heal pain conditions long-term. This applies to the common condition of having a pulled jaw muscle. The integration of preventive self-management training of patients with treatment using a team with technology is a smart model of healthcare– transformative care– that can help the healthcare system recover from its devastating escalation of addiction and disability due to pain in recent years. Transformative care is the basis for the care of patients with pain conditions provided by the integrative pain specialists of the Minnesota Head and Neck Pain Clinic.We offer conservative pain treatment first. SSRIs and antidepressants need careful moderation and oversite to avoid addiction or triggering bruxism.
Why do we use an Interdisciplinary Team?
MHNPC is a model for establishing pain clinics nationally using an interdisciplinary team of pain specialists in Medicine, Dentistry, Nursing, Health Psychology, Physical Therapy, and Health Coaching. The interdisciplinary team is best able to provide successful care for complex by integrating self-management training with evidence-based treatment to help transform patients from pain and illness to health and well-being.
Our clinic is recognized by the American Pain Society designates as a Center of Excellence in pain management and for our Orofacial Pain Specialty expertise.
Self-management focuses on reducing risk factors and enhancing protective actions using brief structured psychophysiological counseling, cognitive-behavioral therapy, and online training. This is combined with short-term use of medical management, physical medicine procedures, injections, and jaw splints that are tailored to the individual needs of the patient.
The specially trained telehealth coach follows up with patients by phone to support the patient in implementing self-management and achieving their goals.
What causes Pain Conditions to Persist and not Heal?
Our goal is to help you resolve your pain long-term.
Pain occurs in cycles with the symptoms caused by diagnoses, which are caused by injury & strain and then made worse by stress. Long-term success can be achieved when we both treat the condition and train you to reduce these causes of pain. The cause of pain conditions is complex. Our goal is to avoid a pain disorder if possible.
Pain cycles involve all realms of your life and are not static and independent but rather are dynamic, evolving, and interrelated processes that involve a set of risk and protective factors that can shift the balance between health and illness.
The factors may be diverse and include the body (e.g., muscle, joint, or nerve conditions, posture, weak tight muscles, lifestyle (habits, repetitive strain, posture, lifestyle, eating, sleep), emotions (depression, fear, anxiety, anger, guilt), society (conflict, relationships, abuse, isolation, social support, secondary gain), mind (attitudes, resilience, expectation, understanding), spirit (purpose, hopes dreams, self-compassion, beliefs), and the environment (risky surrounding, disorganized, unclean, noise, pollution).
We consider it a best practice to avoid opioid prescription use or minimize it as much as possible.
| MN Head and Neck Pain Clinic |
Common Diagnoses and Condition– Muscle pain (myofascial, fibromyalgia-related pain) – Joint pain (arthralgia inflammation) – Joint disorder (disk displaced, arthritis) – Migraine, tension-type headache – Nerve pain (neuropathic, neuralgia) – Ligament or tendon strain – Sleep apnea and snoring issues – Other: |
Pain & Symptoms from Pain Condition– Cluster-type headache – Neck and shoulder pain – Jaw pain, clicking or locking – Ear and facial pain – Tooth and mouth pain – Back and hip pain – Knee and leg pain – Poor sleep and snoring |
|---|---|---|
| Treating and Preventing Chronic Pain |
Causes: Injure or strain tissues– Direct injury and trauma – Repeated strain to muscles and joints – Tensing habits – Postural strain with jaw, sitting, stand – Weak and tight muscles and joints |
Causes: Stress that turns volume up on pain– Lifestyle: sleep, diet, sitting, chemicals – Emotions: depression, anxiety, anger, shame – Social life: conflicts, isolation, work/home stress – Environment: safety, toxicity, side effects – Mind: loss of control, pessimistic, unable to cope – Spirit: low energy, loss of hope, self esteem |
MHNPC Supports National Initiatives to Improve Health Care
The MHNPC pain programs and others like it around the country are also consistent with the Institute of Medicine’s core principles of providing patient-centered care by helping health professionals focus on health care instead of sick care.1-4 When transformative care with robust patient-centered self-management strategies is implemented with all pain conditions, chronic pain, addiction, and care escalation can be prevented.
Thus, health care leaders including the Institute of Medicine, the National Pain Strategy, the Institute for Health Care Improvement, and the Institute for Clinical System Integration have recommended integrating care strategies that engage, educate and empower people in preventing chronic pain and addiction.1-5
The MHNPC also addresses the Institute for Health Care Improvement’s triple aim to improve the patient’s experience of care, enhance the health of the patient, and control the cost of health care.
However, there are many barriers for health professionals to implement transformative care with self-management training. The lack of reimbursement, time burden, and inadequate training skills coupled with the lack of care coordination, fragmented care, poor communication, and conflicting treatments each interfere with patient-centered transformative approaches in clinical practice.
How Does MHNPC Provide Long-Term Cost-Effective Solutions for Pain Conditions?
Every person on our staff is dedicated to treating and preventing your chronic pain.
The MHNPC also has a long tradition of providing a cost-effective solution to chronic pain. The clinicians understand and implement many cost containment strategies in our treatment plans. To achieve cost savings, the clinic developed treatment plans that focus on self-care, self-efficacy, and long-term self-management of their pain while addressing both the physical and mental health needs of the patient.
“Injury to the jaw, the head, or the neck may also cause TMD. Arthritis and displacement of the jaw joint disks can also cause TMD pain. In other cases, another painful health condition such as fibromyalgia or irritable bowel syndrome may overlap with or worsen TMD pain. A recent study by the NIDCR identified clinical, psychological, sensory, genetic, and nervous system factors that may put a person at higher risk of developing chronic TMD.
TMD symptoms can come back during times of stress. It is helpful to be aware of what triggers your symptoms so you can do things to prevent a recurrence.” – Chronic Pain in Temporomandibular Disorders (TMD) by the University of Rochester Medical Center
The clinic focuses on musculoskeletal health including the range of motion, strength, and conditioning to help patients return to normal functioning. The clinic also provides pain patients with a pain home to minimize overutilization of care. All of their pain care needs can either be provided by the team of pain specialists or arranged and coordinated including care with primary care physician, on-call and emergency visits, and phone and e-visits for healthcare support.
The clinic uses specific criteria for imaging, surgery, and pharmaceuticals as indicated and encourages the use of evidence-based medications when possible. The clinic’s focus on long-term care helps prevent chronic pain and its consequences of addiction, disability, and long-term health care costs by empowering patients to self-manage their pain. You can gain relief from a pulled jaw muscle, headaches, neck and should pain at our clinics.
Call our office today and request your appointment: 763-577-2484
References:1. Institute of Medicine. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research. National Academies Press, Washington, DC; June 29, 2011.
2. National Pain Strategy at http://iprcc.nih.gov/docs/DraftHHSNationalPainStrategy.pdf. Accessed on January 10, 2016.
3. Institute for Clinical Systems Improvement. Guidelines for Chronic Pain. https://www.icsi.org/_asset/bw798b/ChronicPain.pdf. Access Feb. 11, 2106
4. Institute for Healthcare Improvement’s (IHI) Triple Aim found at http://www.ihi.org/offerings/Initiatives/TripleAim. Accessed Feb. 11, 2016
5. Lawson K, Whitebird R, Vazquez-Benitez, G, Grossman E, Fricton JR, PACT—A Transformative Self-management Program for Chronic Pain Utilizing On-line Education and Tele-Health Coaching. 2018 International Congress on Integrative Medicine & Health (Abst)
6. Institute for Healthcare Improvement’s (IHI) Triple Aim found at http://www.ihi.org/offerings/Initiatives/TripleAim. Accessed Feb. 11, 2016.