Why Does My Cheekbone Hurt?
By Preetanjali Thakur, BDS, MS
A patient’s guide to understanding the complex causes of cheekbone pain and finding the right diagnosis and treatment options from the specialists at Minnesota Head & Neck Pain Clinic.
“Cheekbone pain” itself is a symptom, not a formal medical condition.
This article will provide an evidence-based overview of the common causes of cheekbone pain to understand when to seek medical care. One such condition that can contribute to cheekbone pain can stem from Temporomandibular joint (TMJ) or masticatory (clenching) muscles.
Within your jaw anatomy, the temporomandibular joint (TMJ) connects the lower jaw (mandible) to the skull. TMJ with masticatory (muscles) allows for complex movements pertaining to daily life like talking, eating, smiling, etc. Your masseter muscle is attached to the cheekbone or zygomatic bone and is responsible for chewing.
When this joint or the supporting jaw muscles are inflamed, injured, or overused, they can lead to cheekbone soreness or discomfort.
Are TMD and Cheek Pain Related?
TMD, or TMJ dysfunction/disorder is a condition that affects the jaw joint and the surrounding muscles that control jaw movements.In fact, cheekbone pain is a classic symptom of a temporomandibular joint (TMJ) disorder. Therefore, pain from these structures can radiate to the cheeks, around the eyes, temples and even the forehead.
Various medical conditions or stress building up over time may interfere with healthy jaw function. This makes accurate diagnosis and tailored treatment crucial for effective management. For example, sprain of a jaw muscle can cause not only jaw pain but also, headaches, earaches, and discomfort in the cheekbones.
Cheekbone pain can come from several sources. Let’s explore the most common ones.
Probable Causes of Cheek Pain
While cheek pain frequently stems from a TMD or myofascial (jaw) issue, pain felt in the cheekbone area may come from other causes too. Most of the time, it is not serious, but sometimes it can be a sign of a condition that needs urgent medical attention.
Additional common causes of cheekbone pain:
- Teeth Grinding (Bruxism): When you persistently grind or clench your teeth, the muscles under your cheeks become overworked. This can lead to sore cheeks and temples due to overworking the jaw muscles. The masseter muscle, a primary chewing muscle, courses from your cheekbone (zygomatic arch) to your jaw. Overworking this muscle due to clenching teeth or grinding can directly cause pain that extends to the cheekbone.
- Sinusitis (Sinus Infection): The largest of your four paranasal sinuses, called the maxillary sinus, is a cavity that is located in your upper jaw (maxilla). The maxilla is located next to the zygomatic or cheekbone. As the maxillary sinus sits just behind the cheekbone, sinus infections can cause pain, pressure, or fullness in the cheeks. This is often present with nasal congestion, facial pressure, or thick nasal discharge.
- Dental Problems: These may include toothache, dental abscess, and periodontal disease, leading to pus and infection in the surrounding area. It is not uncommon to experience cheekbone pain and pain in your teeth directly after a dental procedure. While some cheek and tooth soreness is considered normal, it becomes a concern if this pain continues or worsens after a few days. Dental infections can become serious if not treated, so dental pain with swelling or fever should be checked promptly.
- Trigeminal Neuralgia: This can be a rare cause of cheek pain. The trigeminal nerve is the largest cranial nerve and is responsible for facial nerve functions (both sensory and motor). Disorder of this nerve can cause intense facial pain. Trigeminal neuralgia pain is often an extremely sharp, intense, electric shock-like sensation that is very short-lasting. This contrasts with the achy, pressure, sharp, or dull pain typically associated with TMJ disorders, which is usually aggravated by jaw movements.
- Shingles (Herpes Zoster): Shingles is a painful viral infection and can also affect the nerves of the face, causing pain and a rash along the cheek. Facial pain may start before the rash appears. Shingles is most common on the torso, neck, and back. It is commonly seen on the forehead and can be associated with fever and fatigue. Early treatment with antiviral medication can help reduce symptoms and complications.
- Facial Trauma: A car accident, face-planting fall, sports injury, or facial fracture can cause pain, swelling, and bruising. Facial fractures may involve several bones, such as the orbit, maxilla (upper jawbone), or the cheekbone.
Is Your Cheek Pain Caused by TMJ? If your symptoms align with a TMJ disorder, we’ll help you understand your TMJ treatment options.
Call (763) 577-2484
Less common causes of cheekbone pain:
Other causes of cheek pain may include orbital cellulitis, which is an eye infection and may need immediate care to avoid vision changes and the spread of eye infection. Cheekbone pain may be secondary to tumors or growth. Warning signs include a longstanding lump, unexplained weight loss, or a mass inside the nose. This should be checked by a specialist.
Knowing this, you may wonder where to turn for guidance and accurate diagnoses. We’ll provide you with a bit more information next.
Why Cheekbone Pain is Often Misdiagnosed
- Referred Pain: Cheekbone pain is often a form of “referred pain,” meaning the sensation of pain is experienced in an area of the body that is not the actual source of the problem. For example, the temporomandibular joint (TMJ) sits behind a major nerve that connects to a network of nerves crossing the face, head, and neck, allowing pain to spread throughout these areas, including the cheeks and teeth.
- Overlapping Symptoms: Pain in the cheekbones and teeth can be a symptom of various conditions beyond TMDs, such as sinus infections (sinusitis), dental issues (tooth abscess, toothache, cracked tooth, broken filling, new tooth eruption, periodontal disease), nerve disorders (trigeminal neuralgia, Bell’s Palsy), inflammatory conditions (Giant Cell Arteritis, Temporal Arteritis), or even more serious underlying medical problems like coronary artery disease or tumors.
- Complexity of Orofacial Pain: Orofacial pain is a complex, chronic health condition that is rarely due to a single etiology, but often encompasses multiple, interlinked factors. This complexity, combined with fragmented care involving multiple referrals, can lead to diagnostic delays and patient frustration.
- Mimicry: Muscles in the face can mimic headaches, and vice versa, which can lead to incorrect diagnoses and ineffective treatments if not appropriately differentiated by a specialist.
Self-Reporting of Cheekbone Pain Intensity and Pattern
Understanding how and where the pain manifests helps orofacial pain specialists differentiate it from other potential causes as listed above.
The more specific you can be about your pain, the faster we can pinpoint its cause. Before your visit, take a moment to jot down your experience about your pain level, symptoms, and triggers. Your observations will give us critical clues for an accurate diagnosis.
A Multi-specialty, Interdisciplinary Approach to Managing Cheekbone Pain
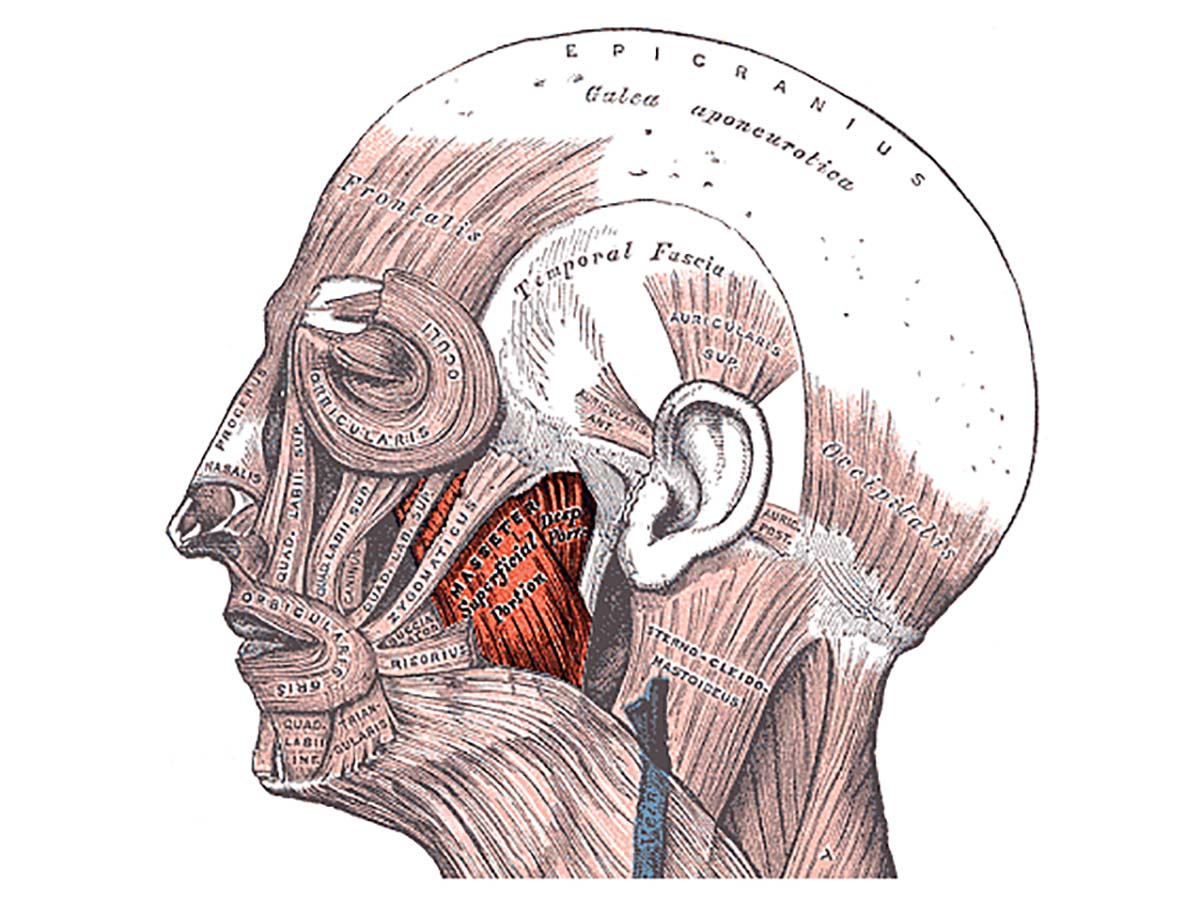
Henry Vandyke Carter and one more author – Henry Gray (1918) Anatomy of the Human Body (See “Book” section below) Bartleby.com: Gray’s Anatomy, Plate 557
Because facial pain can have many possible causes, it’s important to work with a pain specialist who understands these complexities. A thorough and accurate diagnosis often requires a team-based, interdisciplinary approach that may involve multiple specialties working together.
Due to the many possible causes of facial pain and common referral pain in the cheekbone area, it’s essential to have the right pain specialist and an interprofessional approach for correct diagnosis and relevant treatment. This may involve a multi-specialty and interdisciplinary approach.
Most essential is to rule out the red flag symptoms associated with cheekbone pain. This can be rapid, progressive facial swelling, redness, pain with eye movement or visual changes, numbness in the cheek or upper lip, high fever, or even unexplained bruising. Any of these would need urgent evaluation.
TMDs often coexist with other conditions, such as headaches, neck pain, and other forms of facial pain. This complexity means it’s essential to seek medical advice from a niche expert and an integrated care professional.
Cheekbone pain can be classic symptom of TMD
A 2017–2018 data analysis estimated that 4.8% of US adults (11.2 to 12.4 million people) had pain in the region of the TMJ that could be related to TMDs. According to the March 2020 Temporomandibular Disorders: Priorities for Research and Care article:
“TMDs can be transient or long-lasting and may be associated with problems that range from an occasional click of the jaw to severe chronic pain involving the entire orofacial region. Everyday activities, including eating and talking, are often difficult for people with TMDs, and many of them suffer with severe chronic pain due to this condition. ” – National Academies of Sciences, Engineering, and Medicine; Health and Medicine Division; Board on Health Care Services; Board on Health Sciences Policy; Committee on Temporomandibular Disorders
At-Home Care for Cheekbone Pain: What to Do Until Your Appointment
Adults, particularly women in their 50s or 60s can most commonly experience, cheekbone pain, especially in context with jaw symptoms. While you’re waiting for your appointment with an orofacial pain specialist, you can start taking steps at home to feel better and reduce the discomfort.
What can I do at home for immediate relief?
Experiencing persistent cheekbone pain can be frightening and frustrating. While the best course of action is to get an accurate diagnosis from a specialist, here are some safe, practical steps you can take right now to help manage the pain and prevent it from worsening.
Your goal is to reduce inflammation and calm overworked muscles.
- Use Cold and Heat Therapy: For the first 24-48 hours of a new, sharp pain, a cold pack wrapped in a thin towel can help reduce inflammation. Apply it to the sore area for 15 minutes at a time. For a dull, muscular ache that has lasted for a while, moist heat (like a warm, damp washcloth) can help relax the muscles. Apply for 15 minutes.
- Rest Your Jaw: Give your jaw muscles a break. This is one of the most effective things you can do.
- Consider Over-the-Counter Anti-Inflammatories: Medications like ibuprofen (Advil) or naproxen (Aleve) can help reduce both pain and inflammation. However, it’s important to consult with your doctor or pharmacist before taking any new medication, especially if you have other health conditions or take other prescriptions.
- Stress management: Try to manage stress through mindfulness or using coping methods that work with you. We understand that these conditions can be overwhelming and easily contribute to anxiety. However, it may be helpful to focus on relaxation strategies like deep breathing.
- Sleep: Optimum sleep may be helpful for healing. Tissues need time to heal and sleep does wonders to our body and mind in terms of healing and replenishing.
Are there any foods or activities I should avoid?
Yes, absolutely. If you have identified that jaw function is contributing to the pain, resting your jaw will be helpful. It may be most helpful to reduce the stress and strain on jaw. You can be mindful of your daily habits. Like, avoiding hard, chewy, or tough foods (such as steak, bagels, chewing gum, hard granola or bread).
Are there any gentle stretches or exercises I can try?
This is a critical question. Performing the correct exercises is significantly helpful. Your physical therapist can help you establish a personal exercises and stretching routine. However, viewing our podcast on the basics of TMD can have a helpful resource and avoid worsening your symptoms.
- Simple stretch: Until a specialist has identified the source of your pain, you should focus on rest and relaxation. In addition, you can try to identify if you are bracing your jaw or keeping it tight. One simple trick is to remember to have “soft jaw, like the lower jaw is hanging”.
- Focus on Posture: Gently keep your teeth slightly apart and your tongue resting on the roof of your mouth, just behind your front teeth. This is the natural, relaxed position for your jaw and it can help de-program clenching habits. You can also check your head and neck posture—try to keep your head aligned over your shoulders, not jutting forward.”
Is this condition curable, or will I have to manage it forever?
This is a deep and valid concern. While some conditions that cause cheekbone pain are temporary (like an acute sinus infection), chronic conditions like TMD are best thought of in terms of management. The goal of treatment is a significant reduction of pain and the restoration of normal function.
For the vast majority of patients, we can achieve a state where pain no longer interferes with their daily life.
How long does treatment usually take to work?
This depends entirely on the diagnosis and the complexity of your condition. Some patients with muscular strain feel significant relief within a few weeks of starting conservative treatment. More complex cases involving joint issues or long-term chronic pain may take several months of dedicated management to achieve the best results.
Providing you with a realistic timeframe is a key part of our initial consultation.” When we know your medical history, we can map out how the timeline of treatment both in clinic and at home can look like. Research has shown us that people who may suffer with other chronic pain disorders like fibromyalgia may need longer support and pain management.
We are here for you to help you and be supportive. We understand how the autonomic nervous system also plays a role in this presentation.
While at-home care can provide temporary relief, an accurate diagnosis and stepped approach is the key to long-term healing. So that we can not only understand the etiology and cause of the condition but also tailor treatment to address the contributing factors.
How can the Minnesota Head & Neck Pain Clinic Help?
We help people find a lasting solution: you can benefit from the role of a board-certified Orofacial Pain Specialist.
A Orofacial Pain Specialist differentiates between probable causes of cheekbone pain , This may need additional history and tests to understand the duration and character of pain, associated symptoms (nasal discharge, dental symptoms, jaw dysfunction, rash, visual changes).
We will also evaluate for any recent trauma or dental procedures which could have contributed to this presentation. A physical exam will be necessary to rule out swelling and examine for redness, tenderness, cranial nerve deficits, or rash. We may need imaging like (CT or MRI) if we find it will be required for diagnostic clarification.
This approach allows for age-appropriate prioritization of the differential diagnosis and timely identification of serious conditions.
Treatments will be personalized to your condition and treatment approach preferences. We understand why some patients avoid taking medications. Others dislike needles or have lifestyles that prevent them from wearing a bite guard.
The most common cause of chronic facial pain is a non-dental origin. It is widespread but often misdiagnosed.
Through specific muscle palpation techniques, detailed range of motion tests, and, when necessary, advanced imaging, we can differentiate between a muscular TMD issue, a joint problem, a nerve condition, or referred dental pain. This allows us to create an evidence-based treatment plan that is tailored specifically to you.
My Personal Experience Diagnosing Cheekbone Pain and TMJ Dysfunction
A Patient’s Story: Eli’s journey to a successful diagnosis and treatment for pain around her cheekbone.
I was fortunate to work with a lovely 18-year-old who saw me with her mother. Eli started experiencing persistent, dull ache in her ear and sharp pain around her cheekbone that just wouldn’t go away. The patient had already seen numerous specialists—including an ENT, their primary care provider, a dentist, and an occupational therapist—and was exhausted by the process. Moreover, Eli was moving out of state to start college; the impact of this change was dawning on her.
Several doctor visits and imaging ruled out ear and sinus infection but there were no clear answers to her symptoms which seemed to be dull for most part, however, could flare-up from time to time. This also impacted her ability to play soft ball. She was eventually referred to us, orofacial pain specialist at Minnesota Head and Neck Pain clinic.
Here, after a thorough examination and dedicated TMJ related tests, we learned that her symptoms were actually caused by TMJ pain and myofascial pain. She had beginning symptoms of arthritis in her TMJ and associated tight, overworked muscles in her jaw and neck. The pain was being referred from these muscles and TMJ capsule, often aggravated by things like stress, teeth grinding, or poor posture.
With the right treatment, including physical therapy, jaw exercises and relaxation techniques, Eli began to feel relief. We used an oral appliance at night to help with bruxism. Medications were used only for flare-ups. Eli has been asymptomatic for more than 5 years and follows-up with us yearly. She also has the tools and understanding to manage her flare-ups.
Understanding the real cause of her pain helped her take control of it and get back to feeling like herself again.
Seeking Relief for Cheekbone Pain?
If you are experiencing cheekbone pain, an Orofacial Pain Specialist (OFPs) will provide proper diagnosis and treatment options. Minnesota Head & Neck Pain Clinic has a team of board-certified OFPs that determine if the cause is related to TMJ and manage your recovery process. We can determine if your pain is linked to TMD and establish an evidence-based treatment plan to manage your recovery.
Our goal at MHNPC is to be supportive and help you take control and understand your condition to manage this and feel better. I take pride in patient centered care and being sensitive to your needs and helping you navigate to feel better. Nothing makes me more content than being able to help my patients and empower them with useful tools and strategies.
Book Your Appointment Today!
Plymouth: (763) 577-2484
St. Paul: (651) 332-7474
Burnsville: (952) 892-6222
St. Cloud: 763-233-7252
About the author
Preetanjali Thakur, BDS, MS has a Masters in Dental Science and extensive experience that supports her expertise in management of acute and chronic pain disorder treatments. She believes in focusing on self-care, identifying and addressing the contributing factors and working with a team. When needed, Dr. Thakur uses interventional approaches like trigger point injections, and Botox therapy.
Resources:
Eric Matheson, et al., “Temporomandibular Disorders: Rapid Evidence Review,” Jan 2023, https://www.aafp.org/pubs/afp/issues/2023/0100/temporomandibular-disorders.html
Dario Barone, et al., “Odontogenic Orofacial Infections,” Jan 2017, https://pubmed.ncbi.nlm.nih.gov/27930461/
Simon Haworth, et al., “A Clinical Decision Rule to Predict Zygomatico-Maxillary Fractures,” Aug 2017, https://pubmed.ncbi.nlm.nih.gov/28647160/
Giorgio Cruccu MD, et al., “Trigeminal Neuralgia,” Aug 2020, https://www.nejm.org/doi/full/10.1056/NEJMra1914484
Rosenfeld RM, “Acute Sinusitis in Adults,” The New England Journal of Medicine. Setp 2016, https://pubmed.ncbi.nlm.nih.gov/27602668/

